
Healthcare and Ageing | Policy Research Series
《Adding Life to Years: Comprehensive End-of-Life Care for All》
[Full Content (Read Flipbook) - English]
[Full Content (Read Flipbook) - Traditional Chinese]
[Research Summary (Read Flipbook) - English]
[Research Summary (Read Flipbook) - Traditional Chinese]
[Full Content (Download PDF) - English]
[Full Content (Download PDF) - Traditional Chinese]
[Research Summary (Download PDF) - English]
[Research Summary (Download PDF) - Traditional Chinese]
Our Hong Kong Foundation (OHKF) is launching its latest policy advocacy report titled “Adding Life to Years: Comprehensive End-of-Life Care for All.” The report highlights that while Hong Kong's Advance Decision on Life-sustaining Treatment Bill is commendable in promoting end-of-life care (EoLC), this bill alone may not be sufficient to address the full range of care needs. Discussions on EoLC should not be limited to the last 6 to 12 months of one’s life but should be a topic that can be discussed by citizens of all ages. Services should also be expanded beyond medical care to encompass the medical, social, emotional, and spiritual needs of citizens in their final stage of life, ensuring holistic care.
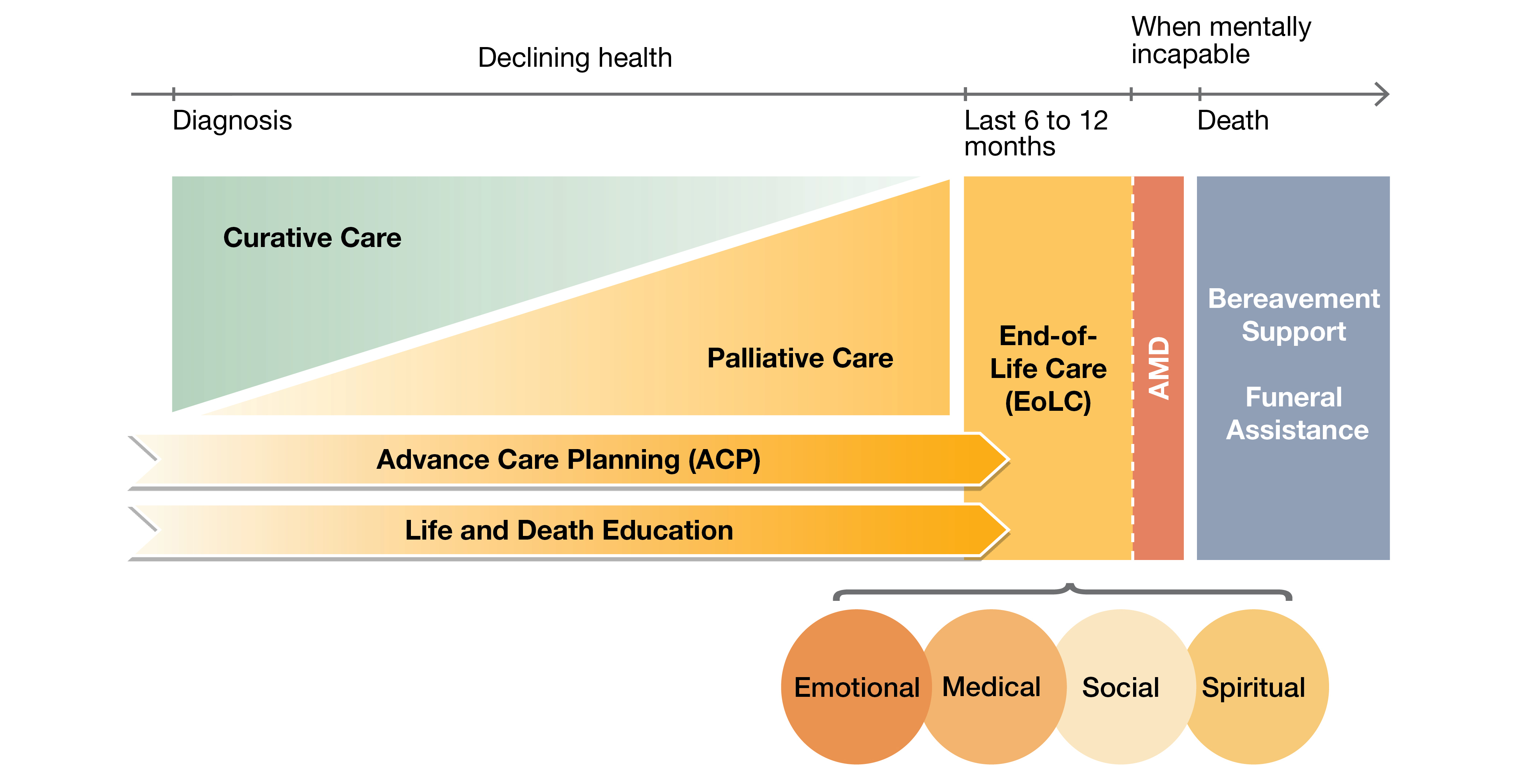
Combining stakeholders’ insights and international case studies, OHKF puts forward 6 policy recommendations across the domains of system, service, and education, through “One Framework, Two Sectors and Three Strategies”, aiming at advancing the development of person-centred, dignified, and coordinated EoLC in Hong Kong:

2022-12-09
《Towards a Fit-for-Purpose Mental Health System》
[(Read Flipbook) Full Report (English Version)]
[(Read Flipbook) Executive Summary (English Version)]
[(Read Flipbook) Executive Summary (Chinese Version)]
[(Download PDF) Full Report (English Version)]
[(Download PDF) Executive Summary (English Version)]
[(Download PDF) Executive Summary (Chinese Version)]
The mental health of the Hong Kong population has been worsening over recent years. Local statistics revealed that one in five Hong Kongers experienced a mental health problem and close to 50% showed depressive symptoms. More importantly, persons with common mental disorders, such as depressive disorder and anxiety disorder, have narrow access to psychological services in the public sector.
The burgeoning mental health crisis points to a pressing demand for ongoing review and enhancements to achieve a reoriented mental health system that adheres to a “fit-for-purpose” vision. To ensure more timely and appropriate access to care, we propose that the mental health system must reorient from its current specialist-centric modality toward a primary care-led service model. Notably, we advocate for leveraging community resources to optimise service accessibility. Multi-disciplinary approaches and cross-sectoral efforts will be crucial in bridging formal care with services available in everyday life settings, such as digital space and workplace.
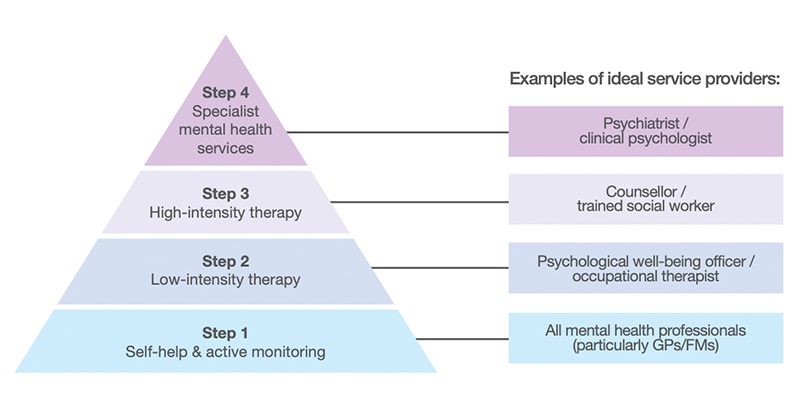
To realise this vision of a community-centric, primary care-led mental health system, efforts are needed to change the existing system structures and to innovate models of care that promote timely access. In particular, we envision the mental health system adopting a stepped care model for psychological therapies that match patients’ needs to the appropriate level of care (Figure 2).
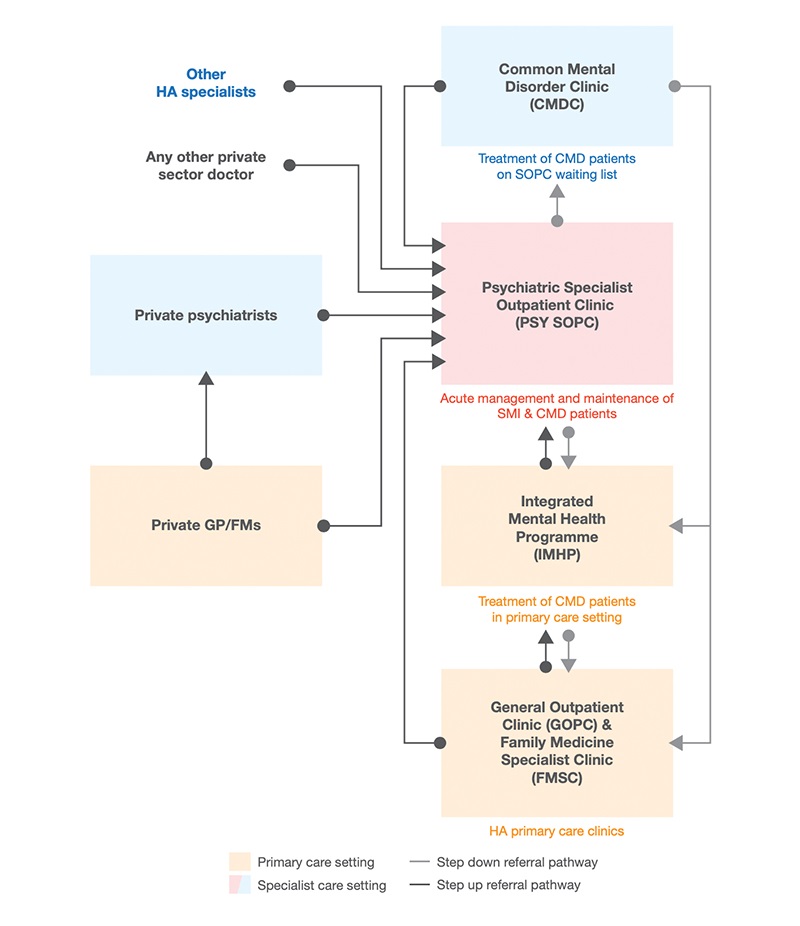
Through interviewing over 70 key stakeholders across medical, social, academic, government and other sectors, conducting two focus groups with mental health services users, and collecting opinions from key service providers in the community through questionnaires, we map the landscape of mental health services, identify the service gaps and challenges in accessing suitable services, and analyse how capacity in the community particularly at the primary care level can be better leveraged for mental health service provision in Hong Kong.
Based on our multi-faceted research, we present five key policy directions:
- Hong Kong must optimise service accessibility through current care models, particularly in non-hospital settings.
- Hong Kong should strengthen formal care models through a stepped care approach for diverse mental health needs.
- Hong Kong should leverage mental health support beyond formal care settings, such as through digital health services and enhancing mental health promotion within the workplace.
- Hong Kong must facilitate system-wide integration through exploring the use of a multidisciplinary data communication platform and adopting a system-wide standardised mental health care protocol.
- Hong Kong should refine the policymaking and policy execution process, particularly in ensuring clear policy implementation plans.
2021-12-20
Strategic Purchasing: Enabling Health for All
[(Read Flipbook) Full Report]
[(Read Flipbook) Executive Summary]
[Download PDF Full Report]
[Download PDF Executive Summary]
While ranked as one of the most efficient health systems globally, Hong Kong is currently facing a population ageing phenomenon and growing burden of chronic conditions. To strengthen the health system against these pressures, emphasis needs to be placed upon pivoting towards healthcare service provision in the community that is integrated across different levels of care, coordinated between specialties and providers, and interfaced with social care. This may be achieved in an integrated, person-centred, primary care-led health system (Figure 1).
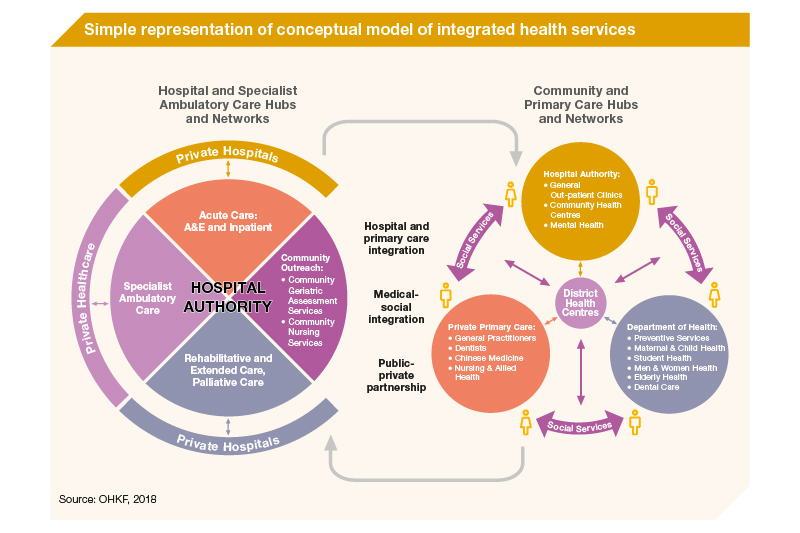
To achieve this new modality and ease the pressure on the public sector health system, it is critical to apply strategic purchasing as a critical health financing lever in governance and health service planning. Concurrently, Hong Kong must consider the use of public-private partnerships (PPPs) as a purchasing instrument to enable better allocation and utilisation of resources to meet population needs.
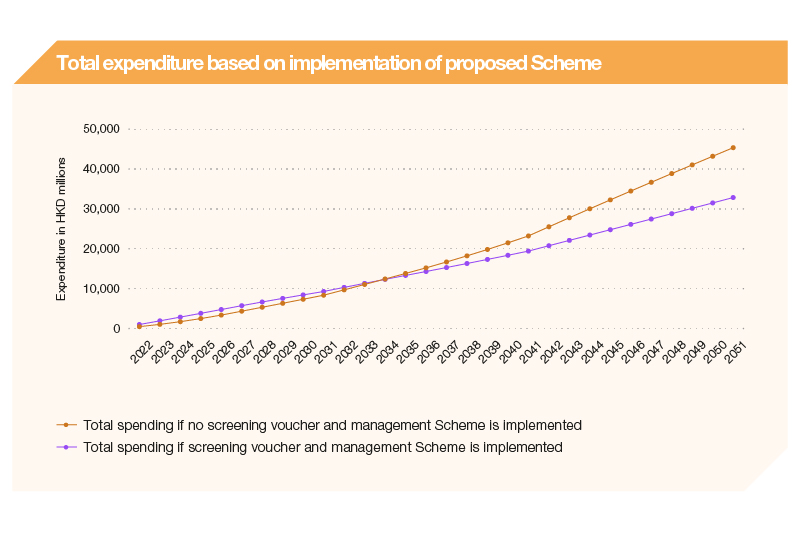
To illustrate the application of strategic purchasing and offer a path forward for developing primary healthcare in Hong Kong, we assessed the feasibility of a Chronic Disease Screening Voucher and Management Scheme (CDSVMS, also addressed as “Scheme”) for three prevalent targeted chronic conditions, namely hypertension, hyperglycaemia (diabetes), and hyperlipidaemia (collectively termed “HDH”) designed based on the perspectives gained from key stakeholders through interviews, and from citizens through a population-based telephone survey. We also projected the economic impact of this Scheme for Diabetes Mellitus (DM) on the health system over the course of 30 years for individuals aged 45 to 54 years of age at the start of the Scheme.
Our research shows that:
1) Stakeholders are supportive of measures to boost access to screening and management of chronic conditions via public-private partnerships designed based on strategic purchasing principles;
2) Over 75% of telephone survey respondents currently without a chronic condition would be willing to join the proposed Scheme;
3) Implementing a screening voucher and management scheme would allow the health system to reduce its expenditures in relation to diabetes care (Figure 2); and
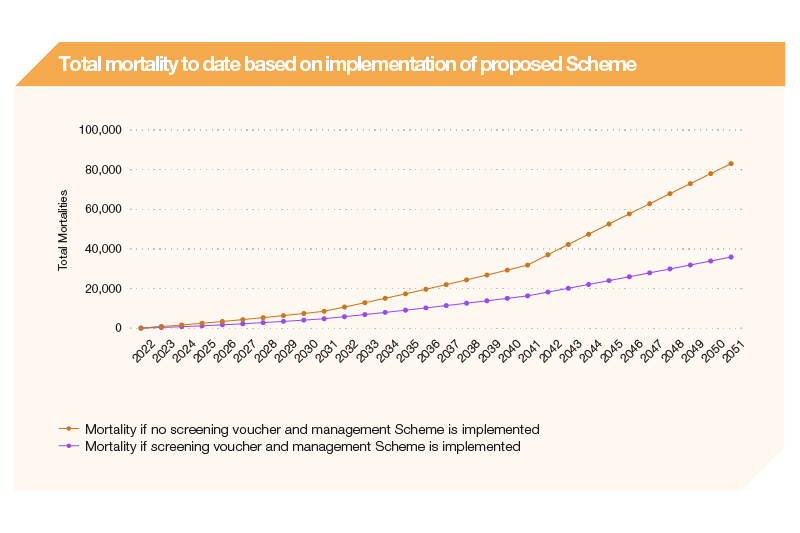
4) Participation in the Scheme will reduce the premature mortality count in relation to diabetes mellitus (Figure 3).
Based on this research, we present four key policy directions:
(1) Hong Kong should apply strategic purchasing and leverage public-private partnerships as a purchasing instrument with a strategic vision for improving primary care accessibility.
(2) Hong Kong should introduce a Chronic Disease Screening Voucher and Management Scheme to enhance primary care access for chronic disease, specifically hypertension, hyperglycaemia (diabetes), and hyperlipidaemia.
(3) The Government must apply key policy dimensions of strategic purchasing to the Scheme, which include: population health, citizen empowerment, strengthening government stewardship and capacity, developing effective purchaser and provider orgnaisations, and incorporating cost-effective contracting.
(4) Health system strategic purchasing should be implemented for achieving an integrated care system to enable health for all, across the health system level (macro), purchaser-provider healthcare delivery system (meso), and person journey of healthcare delivery (micro).
2021-12-1
Building an Age-Friendly City – Embedding Gerontechnology Into Everyday Life
[(Read Flipbook) Full Report]
[(Read Flipbook) Executive Summary]
[Download PDF Full Report]
[Download PDF Executive Summary]
In 2017, Our Hong Kong Foundation published the city’s first gerontechnology report, which identified 24 gaps representing key opportunities and challenges facing Hong Kong’s gerontech ecosystem at the time. To assess the degree of improvement of these gaps and explore how to further develop Hong Kong's gerontech ecosystem, OHKF was commissioned by the SIE Fund’s Gerontechnology Platform to publish a new report entitled “Building an Age-Friendly City – Embedding Gerontechnology Into Everyday Life.”
Back in 2017, Hong Kong’s gerontech ecosystem was very fragmented. In addition to there not being many suppliers, there were few gerontech products and services available on the market, and these products were not reaching target users. Yet, due to the increase in Government and industry initiatives from the past few years, we have seen an increase in the number of suppliers. Hong Kong’s gerontech ecosystem has become more integrated, enabling more end-users to access and use gerontech. While these are positive signs, we believe more can be done. As such, the Report proposes a series of policy recommendations in five key areas, namely related to supply-side, demand-side, infrastructure, investment, and talent development.
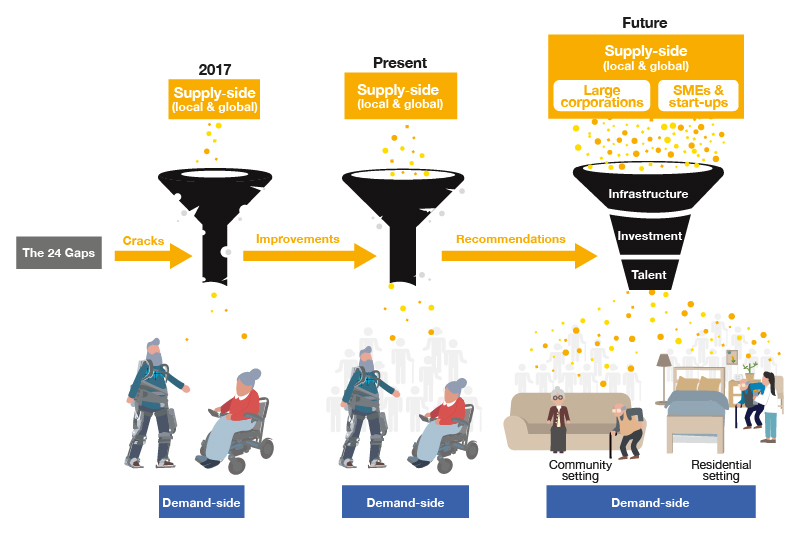
To help supply-side stakeholders, we recommend increasing the opportunities for them to receive user feedback and easing import and export process. For demand-side stakeholders, we recommend extending the existing Innovation and Technology Fund for Application in Elderly and Rehabilitation Care to 100% privately funded elderly homes, as well as extending the coverage of the Elderly Health Care Voucher and Community Care Service Voucher to enable elderly to procure gerontech.
Turning to infrastructure, we recommend the Government to set up a "Gerontech Corner" in District Health Centres to enable elderly and persons with disabilities to more easily access gerontech in their local neighborhoods. We also recommend the Government to extend home modification schemes currently available to elderly and persons with disabilities living in public housing to those living in private housing. Finally, we hope that the Government will attract more parties to grow the gerontech ecosystem. We recommend the Government to seek more gerontech public-private partnership opportunities, particularly through the innovative “Pay-for-Success” financing model. We also recommend the Government to develop more gerontech talent through Qualifications Framework-recognised gerontech professional skill training and robust knowledge transfer-related university policies.
2021-05-27
"Fit to Practise: Reviving the Role of Non-locally Trained Doctors to Strengthen Hong Kong’s Doctor Workforce Today for a Better Tomorrow" Healthcare Research Report
[(Read Flipbook) Full Report]
[(Read Flipbook) Executive Summary]
[Download PDF Full Report]
[Download PDF Executive Summary]
Hong Kong is renowned for its efficient health system and enviable for its population’s long life expectancy, but it is plagued by a longstanding doctor shortage crisis. Unless quick action is taken to address this problem, the doctor shortage gap will continue to widen, with a projected shortfall of 1,610 doctors by 2030, according to the Government’s 2020 Healthcare Manpower Projection. This contributes to potentially dangerous delays in diagnosis, treatment, and management of health conditions.
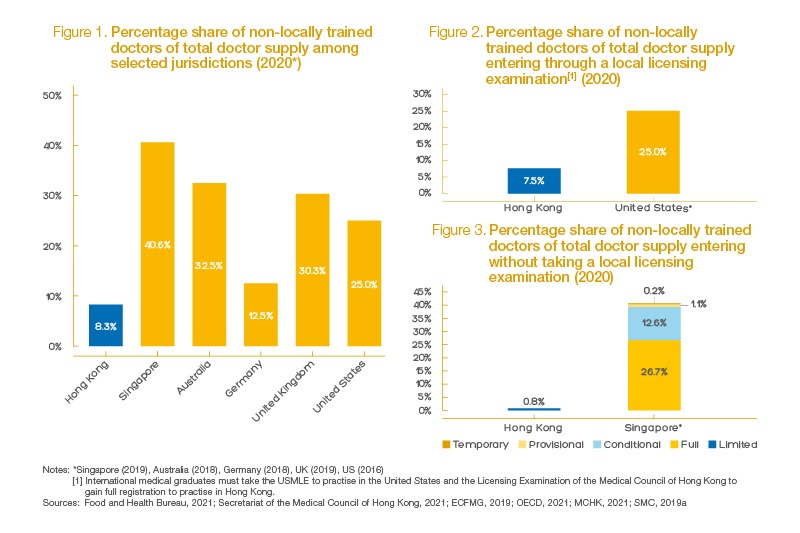
Although the Government has taken a multifaceted approach to increase Hong Kong’s doctor supply, Hong Kong has yet to fully leverage a non-locally trained doctor workforce, which is a missed opportunity to relieve the doctor shortage crisis holistically and effectively. Our research reveals that Hong Kong’s policy efforts to encourage the practice of non-locally trained doctors fall behind those in similarly developed economies such as Singapore and the United States. Hong Kong’s policies around internship placements, training, accreditation and career progression for non-locally trained doctors need to be improved substantially to provide fairer opportunities for non-locally trained doctors.
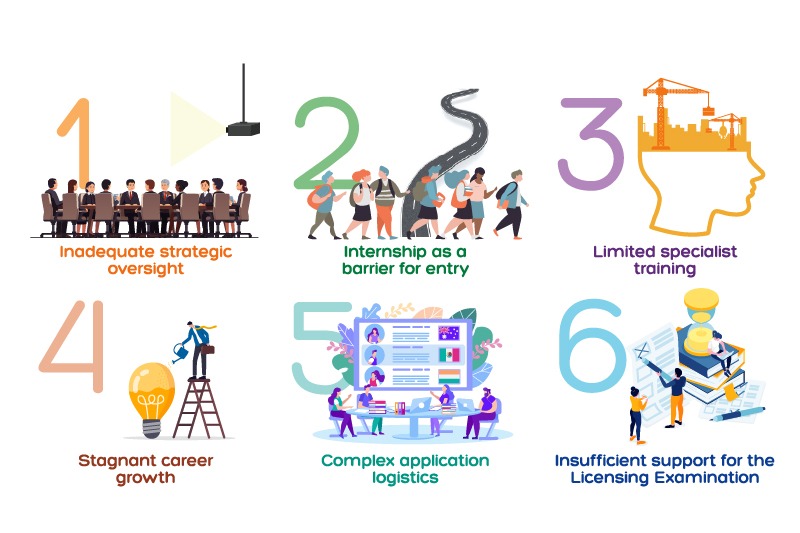
As part of a multi-pronged approach necessary to alleviate the doctor shortage crisis and inspired by exclusive interviews with non-locally trained doctors practising in Hong Kong, we put forth six policy recommendations in response to the six key challenges, so that non-locally trained doctors’ talents can be fully leveraged to provide immediate relief to the local health system:
- Improve governance: 1) Hong Kong must strengthen its governance and strategic vision in health workforce.
- Facilitate registration, internship, training, accreditation, and career progression: 2) Hong Kong can consider providing internship placements and a structured career path for non-locally trained doctors 3) Hong Kong should strengthen its investment in specialist training; 4) Hong Kong must capitalise on and nurture valuable human capital.
- Increase efficiency and equity: 5) Relevant authorities in Hong Kong including the Medical Council of Hong Kong should adopt the Electronic Portfolio of International Credentials to streamline examination application and medical registration procedures; 6) Hong Kong should conduct a review of the Medical Council of Hong Kong Licensing Examination to uphold fair assessment standards.
For specifics, please refer to the full report.
2019-12-16
Fostering Medical-social Collaboration in Achieving Quality End-of-life Care
[(Read Flipbook) Executive Summary]
[(Read Flipbook) Presentation Slides (Chinese version)]
[Download PDF Executive Summary]
[Download PDF Presentation Slides (Chinese version)]
Our Hong Kong Foundation has released the results of a public opinion poll on community end-of-life care services in an advocacy paper entitled "Fostering Medical-social Collaboration in Achieving Quality End-of-life Care". With a laudable life expectancy that ranks top in the world, Hong Kong’s population is ageing rapidly. Greater longevity and the steep increase in co-morbidity in the elderly population have called for increased territory-wide attention on not just the quality of life, but also of death. Yet, our current health system is treatment-focused and hospital-centric, while services are fragmented. Public hospitals are constantly over-burdened in which palliative care development has failed to catch up with the rising needs of citizens. Through understanding public perception and practice related to end-of-life care services in local communities (outside of hospital settings), our study concludes that focusing on end-of-life care at the community level is vital . Key development areas of end-of-life care in Hong Kong include: enhancing public education and advocacy, improving current services in community settings and reorienting development towards primary care level. Echoing our ‘Fit for Purpose: A Health System for the 21st Century’ research report, community resources need to continuously be leveraged upon as we shift care burden from our currently overstretched public hospitals into the community. Our health system should take on a holistic approach in health service provision so that needs of individuals are consistently met throughout the entire life course, including the final stages of life, as we facilitate a better and more dignified end-of-life journey for all Hong Kong citizens.
2019-10-4
An Advocacy Study on "Health System Capacity Constraints- The Severe Shortage of Doctors in Hong Kong Public Hospitals"
[(Read Flipbook) Advocacy Study (full version)]
[(Read Flipbook) Advocacy Study (simplified version)]
[(Read Flipbook) Leaflet]
[(Download PDF) Advocacy Study (full version)]
[(Download PDF) Advocacy Study (simplified version)]
[(Download PDF) Leaflet]
Our Hong Kong Foundation has released its advocacy study today, entitled " Health System Capacity Constraints- The Severe Shortage of Doctors in Hong Kong Public Hospitals". The study points out that the severe shortage of doctors contributes to the challenge of timely access to quality healthcare for our local population, particularly in the public sector. This longstanding issue is exacerbated by a rapidly ageing population and growing burden of chronic diseases that represent an ever-increasing demand for healthcare services, and immediate action needs to be taken. The study points to the urgent need to be more receptive towards augmenting the role of foreign-trained doctors in our health system. Specifically, procedures currently in place that allow for foreign-trained doctors to practice in Hong Kong should be reviewed to attract more well-qualified foreign-trained talent to join our healthcare workforce to relieve our shortage of doctors, particularly in our public hospitals.
2018-11-30
Fit for Purpose: A Health System for the 21st Century
Our Hong Kong Foundation (hereafter referred to as the "Foundation") has published a report today on Hong Kong’s health system, entitled "Fit for Purpose: A Health System for the 21st Century". The report points out that Hong Kong's health system is not fit to meet 21st century challenges. To tackle fundamental underlying problems, system-level changes are necessary to transform the system from its current emphasis on acute hospital-centric care to one that is integrated, person-centred and puts emphasis on primary care for all citizens of Hong Kong so that comprehensive and continuous care could be provided over their life course. The research report recommends policy options covering three key areas including: 1) enabling person-centred care; 2) achieving primary care-led integrated care; and 3) putting in place health governance levers to enable the transformation process.
2017-06-12
Gerontechnology Landscape Report
Our Hong Kong Foundation has released its research report on gerontechnology in Hong Kong, entitled “Gerontechnology Landscape Report”. The landscape report studies and identifies the relevant stakeholders and the different gaps and difficulties within the gerontechnology ecosystem. A selection of available gerontechnology products and services in Hong Kong are also explored within four categories: healthcare, food, living and transport.
With a rapidly ageing population and a declining labour force, technology within the elderly health care sector is becoming increasingly important. Gerontechnology could be the key to tackling the problems ahead, and allow Hong Kong to turn these challenges into a golden opportunity to transform into a technologically advanced city, hence benefit seniors and their caregivers.
2016-12-09
Aging Society Research Report
Our Hong Kong Foundation has published the first Aging Society Research Report, entitled ‘An Investment for the Celebration of Aging’. The research report recommends key policy options, namely the creation of a Chronic Disease Management Voucher Scheme and a Health-Enabling Network, the establishment of collaborative governance and social capital, and the use of technology, to unleash the potential of a growing older population and generate overall greater well-being throughout Hong Kong.
Stakeholders of each and every sector will need to collaborate and invest in Hong Kong’s physical, social and political institutions for an age-enabling environment so that everyone, regardless of their age and ability, can celebrate their lives.



